Last week, shortness of breath after exertion led to an urgent visit to the doctor. What I first thought was a recurrence of bronchitis turned into an up close a personal encounter with medical technology and a much-maligned system that at its best works very well indeed. It also left me convinced that, while I still doubt that electronic medical records can be the big money saver that advocates claim, EHR can definitely improve the quality of care and save lives.
I have been a member of Kaiser Permanente Mid-Atlantic for many years and my experience began in urgent care at a Kaiser facility about five minutes from home. After I described my symptoms, they put me on oxygen and began tests. When blood tests suggested the possibility of a clot but a chest x-ray was inconclusive, they gave me an injection of the anticoagulant Lovenox and shipped me by ambulance to a second Kaiser facility equipped with a CT scanner.
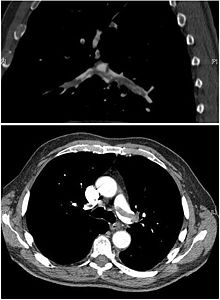
Because Kaiser has an excellent EHR system (developed at great cost and after a couple of painful false starts) and requires doctors and nurses to document everything in the system, the staff at Kaiser Capitol Hill knew everything that had happened at my neighborhood facility. They continued the tests and treatment and when the CAT scan showed a dangerous pulmonary embolism, they decided I belonged in the hospital.
Another ambulance ride took me to Holy Cross Hospital in Silver Spring where I spent an uncomfortable day and a half being poked, prodded, tested, and generally well cared-for. Holy Cross is heavily used by Kaiser and is hooked into their system, so again the staff instantly knew everything that had been done. (It was also kind of cool to get the results of tests run the night before on my iPad, including the good news that a cardiac enzyme test for possible heart damage was negative, while lying on my hospital bed.)
I realized how useful the EHR system really was when I got a new roommate after I had been declared stable and was waiting for my wife to come fetch me. A man in his 80s and apparently suffering from some level of dementia was brought in, though neither he nor the hospital staff seemed to know exactly why (there is absolutely no privacy in a hospital room.) He remembered that he had suffered an allergic reaction to penicillin during World War II, but wasn’t sure what led to his being taken to the hospital. Without good access to his medical records, the nurse was having a bad time just trying to figure out what meds he was on. Both he and the hospital staff were at a huge disadvantage because they had no history to work with.
It’s going to take a while, and a lot of money, before the U.S. health care system comes close to matching the EHR systems of organizations such as Kaiser and the Veterans Administration. Both have the enormous advantage that their doctors are employees, not affiliates, and therefore can be required to use the system. But building a national EHR system is vital work, and the much-maligned Affordable Care Act should help spur things along.
As for me, I’m happy to say that I’m doing well. The anti-clot treatment seems to be working as the shortness of breath is gone. I’ll be on blood thinners for some months and I’ll be a lot more careful about flying once I get back in the air. Flying, especially long flights in cramped conditions, are a well known risk factor for the deep vein thrombosis that leads to pulmonary emboli and the nine legs I flew, including two of more than 12 hours, in the month before I landed in the hospital, certainly didn’t help.
On a personal note, I want to thank the urgent care staffs of Kaiser Permanente Kensington and Capitol Hill and the staff of the monitoring unit at Holy Cross Hospital for the treatment I received during this adventure. I don’t think I could have asked for better care.

Steve, good to hear it worked for you.
Several years ago I did a programing stint for a medical imaging records company. Having a background in usability I went and looked it up. In many real world situations you are still better off with paper. Why? Paper often stays with you (often they literally attach files to the end of your bed.) Electronic records are still misfiled (name misspelled, or two people with similar names) systems have incompatible. In short electronic records are no panacea and are just as often a much more expensive alternative that works no better. Like all tools in places that they are used well, they work well, in places that they are not, not so much. I personally don’t believe electronic records will work well until the industry starts making sure a thumb drive goes with the patient so that a copy of their records goes with them. That is not a perfect solution either and will require open formats and privacy standards that are not yet universal or ideal.
No one knowledgeable says this will be easy. The technical issues are daunting, the human issues are worse. As I note in passing, it’s no accident that the most successful implementations to date have involved institutions where doctors are employees rather than independent agents. Without full compliance from the docs, none of this is going to work, and that compliance is difficult to achieve.
There are a couple of problems with the thumb drive approach. One is security/confidentiality of the information, which would certainly have to be HIPAA-compliant. Encryption would work, but key management becomes a nightmare. The second issue is that in a situation such as the one I was in, you really need something close to real-time sharing; for example, some of the labs were still being run when I was transferred from once facility to another. You need a way for the data to follow the patient.
The US Patriot Act issues may be even the worst of all.
EMR will be an expensive fiasco for many reasons. First the are no standards for compatiability and many systems will have to be replaced periodically so that vendors can make more money.
Computer records are loaded with boilerplate data that is useless and that will bury important information in minutae. Paper records also contain useless info also but it is easier to add boilerplate with EMR.
The major advantage of computerized records is to actually store the real data such xray images but most only store the written report which can be wrong and misleading.
EMR if necessary could be stored on a flash drive and given to the patient but this would be too simple.
Most people do not know that it may initially cost up to 50K per physician to implement an EMR perhaps driving up the cost of medicine.
Thank you for great article. I look forward to the continuation.
We always follow your beautiful content I look forward to the continuation.